Imaging Tests for Lower Back Pain: Choosing Between X-Ray, MRI, and CT Scan
Lower back pain is a common ailment that affects millions of people worldwide, often leading to the need for diagnostic imaging to determine the underlying cause. Understanding the various imaging tests available—X-Ray, MRI, and CT Scan—can help patients make informed decisions about their healthcare. Each imaging modality has its unique strengths and weaknesses, making it essential to choose the right one based on specific symptoms and conditions. This article will explore the primary imaging options for lower back pain, detailing how each test works, when they are recommended, and their respective advantages and risks. By the end, readers will have a clearer understanding of how to select the best imaging test for their needs.
However, it’s important to consider that diagnostic imaging for low back pain is often utilized more frequently than clinical guidelines recommend, potentially leading to unnecessary radiation exposure and adverse patient outcomes.
X-Ray, MRI, CT Use & Outcomes for Low Back Pain
Low back pain is one of the most common and disabling health problems in Canada and internationally. In most cases, low back pain is a benign, self-limiting condition that can be managed with little diagnostic investigation or treatment. Yet contrary to clinical practice guideline recommendations, diagnostic imaging (here meaning X-ray, MRI, CT) is commonly used in the assessment of low back pain. Diagnostic imaging is of limited value in most cases, exposing patients to unnecessary radiation and leading to increased health services use and worse patient health outcomes.
Development of a clinical decision support tool for diagnostic imaging use in patients with low back pain: a study protocol, JA Hayden, 2019
X-Ray
X-Ray imaging is a quick and painless procedure that primarily focuses on visualizing bone structures. It works by passing a small amount of radiation through the body, which is absorbed differently by various tissues, creating an image on film or a digital sensor. This method is particularly effective for early detection of bone-related issues, such as fractures or degenerative changes in the spine. However, X-Rays have limitations, as they are not as effective in visualizing soft tissues, such as muscles, ligaments, and intervertebral discs.
Indeed, research highlights the varying diagnostic capabilities of different imaging modalities for spinal injuries.
X-Ray, CT, MRI Sensitivity for Spinal Injury Detection
However, the reported sensitivity for plain radiographs to detect spinal injuries is unclear and specificity of CT scans and MRI have reported up to 100% sensitivity for CT scans (21,22).
Cervical spine trauma–Evaluating the diagnostic power of CT, MRI,
X-Ray and LODOX, N Rutsch, 2023
MRI (Magnetic Resonance Imaging)
MRI is a non-invasive imaging technique that uses strong magnetic fields and radio waves to generate detailed images of soft tissues in the body. It is particularly beneficial for evaluating conditions affecting the spinal cord, nerves, and soft tissues surrounding the spine. Unlike X-Rays, MRI does not involve radiation exposure, making it a safer option for many patients. However, MRI scans are generally more expensive and may take longer to perform compared to X-Ray imaging.
CT Scan (Computed Tomography)
CT scans combine X-Ray technology with computer processing to create cross-sectional images of the body. This imaging modality is especially useful for detailed bone imaging and is often employed in emergency situations due to its speed. CT scans can provide a comprehensive view of the spine and surrounding structures, making them valuable for diagnosing complex conditions. However, they do involve exposure to radiation, which is a consideration for both patients and healthcare providers.
Summary
When it comes to diagnosing lower back pain, each imaging test has its unique advantages and limitations. X-Rays are ideal for quick assessments of bone injuries, while MRIs excel in providing detailed evaluations of soft tissue injuries. CT scans are preferred for rapid imaging in emergencies, particularly when detailed bone imaging is required. Understanding these differences can help patients and healthcare providers make informed decisions about the most appropriate imaging test for their specific needs.
What Are the Primary Imaging Options for Lower Back Pain?
The primary imaging options for lower back pain include:
- X-Ray: Best for identifying bone fractures and alignment issues.
- MRI: Ideal for assessing soft tissue injuries, such as herniated discs and nerve compression.
- CT Scan: Useful for detailed bone imaging and complex cases, especially in emergency settings.
How Does X-Ray Imaging Diagnose Lower Back Conditions?
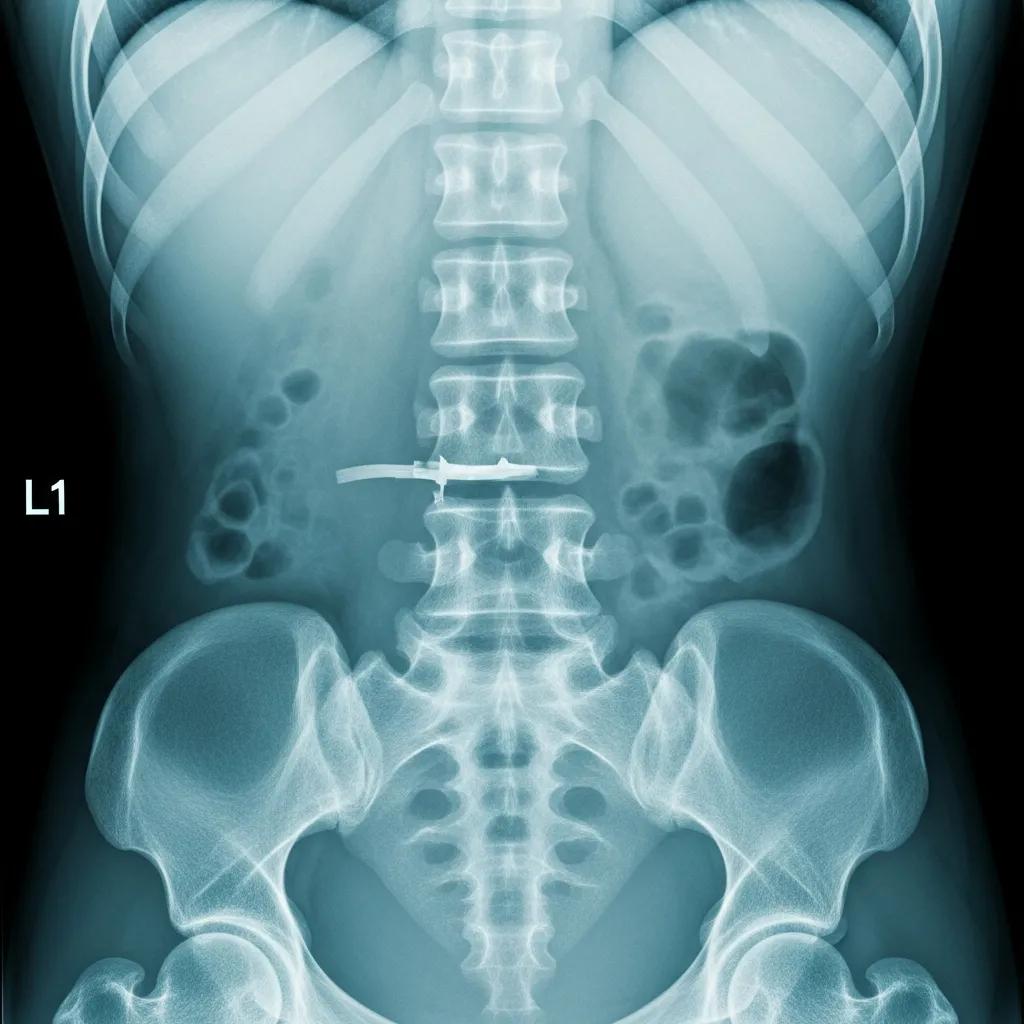
X-Ray imaging diagnoses lower back conditions by providing clear images of the bony structures of the spine. Patients typically undergo a simple preparation process, which may include removing clothing or jewelry that could interfere with the imaging. X-Rays can identify conditions such as fractures, arthritis, and spinal alignment issues. Compared to MRI and CT scans, X-Rays are quicker and less expensive, making them a common first step in the diagnostic process.
When Is MRI Recommended for Back Pain Evaluation?
MRI is recommended for back pain evaluation when there is a suspicion of soft tissue damage, such as herniated discs or spinal stenosis. It is particularly useful for patients experiencing neurological symptoms, such as numbness or weakness in the legs. The absence of radiation exposure makes MRI a safer option for repeated imaging, especially in younger patients or those requiring ongoing evaluation.
While MRI is often highlighted for its soft tissue detail, research has also explored the comparative diagnostic accuracy of various imaging techniques, including CT and myelography, for conditions like lumbar disc herniation.
CT, MRI, Myelography Accuracy for Lumbar Disc Herniation
We found 14 studies, all but one done before 1995, including 940 patients. Nine studies investigated Computed Tomography (CT), eight myelography and six Magnetic Resonance Imaging (MRI). The prior probability of LDH varied from 48.6 to 98.7%. The summary estimates for MRI and myelography were comparable with CT (sensitivity: 81.3% (95%CI 72.3–87.7%) and specificity: 77.1% (95%CI 61.9–87.5%)). The quality of evidence was moderate to very low.
Diagnostic accuracy of diagnostic imaging for lumbar disc herniation in adults with low back pain or sciatica is unknown; a systematic review, RM van Rijn, 2018
How Do CT Scans Contribute to Lower Back Pain Diagnosis?
CT scans contribute to lower back pain diagnosis by providing detailed cross-sectional images of the spine and surrounding structures. They are particularly effective in identifying complex fractures, tumors, or infections that may not be visible on X-Rays. The speed of CT scans makes them an excellent choice in emergency situations where rapid diagnosis is critical. However, the radiation exposure associated with CT scans is a consideration that must be weighed against the benefits.
What Are the Advantages and Risks of CT Scans for Back Pain?
CT scans offer several advantages for diagnosing back pain, including:
- Speed: CT scans can be performed quickly, making them ideal for emergency situations.
- Detail: They provide high-resolution images that can reveal complex conditions.
- Comprehensive: CT scans can visualize both bone and soft tissue structures.
However, there are risks associated with CT scans, primarily due to radiation exposure, which can increase the risk of cancer over time. Additionally, CT scans may not be as effective in visualizing soft tissue compared to MRI.
In Which Cases Is CT Imaging Preferred Over Other Modalities?
CT imaging is preferred over other modalities in cases where rapid diagnosis is essential, such as:
- Acute Injuries: When immediate assessment of fractures or trauma is needed.
- Complex Conditions: For detailed evaluation of tumors or infections.
- Emergency Situations: When time is critical, and quick imaging is necessary.
How to Choose the Best Imaging Test for Your Lower Back Pain?
Choosing the best imaging test for lower back pain involves considering several factors, including:
- Type of Injury or Condition: Understanding whether the issue is bone-related or involves soft tissues.
- Symptoms: Evaluating the presence of neurological symptoms can guide the choice of imaging.
- Cost and Availability: Considering the financial implications and accessibility of each imaging modality.
For those seeking imaging services, X-Ray Docs specializes in X-Ray, MRI, and CT scan services, providing comprehensive diagnostic imaging tailored to individual needs.
What Factors Influence the Selection Between X-Ray, MRI, and CT Scan?
Several factors influence the selection between X-Ray, MRI, and CT scan, including:
- Clinical Indications: The specific symptoms and suspected conditions guide the choice of imaging.
- Cost Considerations: X-Rays are generally less expensive than MRIs and CT scans.
- Patient Circumstances: Factors such as age, medical history, and previous imaging can impact the decision.
How Do Imaging Results Impact Treatment Planning?
Imaging results play a crucial role in treatment planning for lower back pain. They help healthcare providers determine the underlying cause of pain, which can influence the choice of treatment options. For instance, if an MRI reveals a herniated disc, a physician may recommend physical therapy or surgery, while an X-Ray showing a fracture may lead to a different treatment approach. Understanding the implications of imaging results is essential for effective patient management.
How to Book and Prepare for Lower Back Pain Imaging at X-Ray Docs?
Booking and preparing for lower back pain imaging at X-Ray Docs is straightforward. Patients can schedule an appointment by contacting the facility directly. It is essential to bring any necessary documentation, such as referrals or insurance information. Preparation may vary depending on the type of imaging, so patients should follow specific instructions provided during the booking process.
What Is the Process for Scheduling an Imaging Appointment?
The process for scheduling an imaging appointment typically involves:
- Choosing a Booking Method: Patients can book via phone or online.
- Preparing for the Appointment: Gather necessary documents and information.
- Informing Staff About Medications: Disclose any medications or allergies to ensure safety during imaging.
How Should Patients Prepare for Each Imaging Test?
Preparation for each imaging test may vary:
- X-Ray: Patients should remove any metal objects and wear comfortable clothing.
- MRI: Patients may need to avoid food or drink for a few hours before the test and inform staff about any implants or devices.
- CT Scan: Patients may be advised to drink plenty of fluids and avoid certain medications prior to the scan.
Understanding these preparation steps can help ensure a smooth imaging experience and accurate results.